How to Cite | Publication History | PlumX Article Matrix
Mohammad kazemian1, Seyed Hossein Fakhraee2, Korosh Kosari3*
1Neonatologist, Shahid Beheshti University of Medical Sciences, Tehran, Iran 2MD-FAAP, Neonatologist, Shahid Beheshti University of Medical Sciences, Tehran, Iran 3Neonatologist, AJA University of Medical Sciences, Tehran, Iran
ABSTRACT: Transportation of unstable newborn to well equiped NICU is very important in managing such patients. So investigation the condition of transportation is very important for revealing the probable problem. The aim of this study is to investigate the condition and problems of the newborn infants before and during transportation to Mofid children’s Hospital NICU as a one of major referal center in Iran. This is a cross sectional study conducted in Sep 2010 to Sep 2011. In this period all newborn transported to NICU ot Mofid hospital were enrolled. For each newborn a questionnaire consisting of question about demographic, condition of transportation, time of transportation, drugs and other treatment measurs were filled. Totally 211 patients were enrolled. In 58(27.5%), 123 (58.5%), and 41 (19.4)% a MD, a nurse or a technician respectively accompanied the newborn in transportation. In 52(24.6%) cases had tracheal tube and In 159 (75.4) cases did not have it. In 167(70.1%) were stable were reached to NICU. In 11 (5.2) cases were hypothermic. In 31 (14.7%) cases were cyanotic. There were no significant relation between person of transporter with stability of newborn. Unstable newborn were transported by physician more than nurses and technicians. In stable group more people passed the newborn CPR workshops but this difference was not significant statistically. In spite of progress in transportation condition recently, better specialized training for newborn transportation can improve transportation yet. It is necessary to register transportation data more precisely.
KEYWORDS: Newborn Transportation; NICU; Hospital
Download this article as:| Copy the following to cite this article: Kazemian M, Fakhraee S. H, Kosari K. Study of the Condition and Problems of the Newborn Infants Before and During Transportation to Mofid Children’s Hospital NICU. Biosci Biotech Res Asia 2015;12(2) |
Introduction
Healthcare activities in every country are assessed by the rate of newborns and mothers’ deaths during the pregnancy or thereafter 1. One important factor with great effect on mortality of newborns is the appropriate way of transportation from the birth place to neonatal unit or NICU.2
It has been estimated that in 50% of high-risk pregnancies transportation of mother is impossible before the delivery. In such conditions transportation of the newborn must be carried out by a highly trained team 3. In a study by Hood et al, it was shown that the mortality is 60% higher when the newborn is transported by an untrained team 4. In these cases hypothermia and acidosis are the most common events5.
Development and improvement of NICUs and inter-hospital transportation services for severely ill newborns are important factors in reducing mortality and morbidity6. About 40 years earlier women and newborn specialists found that newborn outcomes were better when received treatment in level 3 centers 7. However, the goal of newborn transportation is not the physical transfer of the subject with any conditions and any equipment, but it is the reduction of death rate of newborns by means of stabilizing the general conditions before the transportation and maintaining those conditions during, and after 8.
Considering the above mentioned points and the danger of parturition and high susceptibility of newborns, improvement of medical care during the transportation to specialized centers is a must in order to reduce their mortality, intra-transportation side effects, and transportation duration 9. Thus, the existence of a newborn transportation system in the trained team is a necessity for making developed equipment and specialized centers accessible to newborns.
Any form of intervening and inappropriate decisions during the newborn transportation can result in unwanted outcomes such as pain, increased mortality, increased expenses, side effects, and time waste 10. Thus, the presence of trained personnel, appropriate equipment and vehicles, and transportation protocols are necessary during the transportation to level 3 centers 11. Therefore, assessment of the present conditions in newborn transportation has an important effect on determination of advantages and disadvantages of this process and future planning. This study aims to investigate the condition and problems of the newborn infants before and during transportation to Mofid children’s Hospital NICU as one of the major referral centers in Iran.
Materials and methods
This is a cross sectional study conducted in Sep 2010 to Sep 2011. In this period all newborn transported to NICU ot Mofid hospital were enrolled. For each newborn a questionnaire consisting of question about demographic, condition of transportation, time of transportation, drugs and other treatment measures were filled. In the end, collected data were reported in the form of descriptive statistics using the mean and standard deviation for quantitative data, and frequncy and relative frequency for qualitative data. Chi-squred test was used to compare the means and relations.
Results
From the total of 211 questionnaires 119 (56.4%) were filled by male participants and 92 (43.6%) by females. The qualitative and quantitative information of subjects is shown in tables 1 and 2 respectively.
Table 1: Qualitative variables of subjects
| variable | frequency | Relative frequency | |
| Transporter, physician | 58 | 27.5% | |
| Transporter, nurse | 123 | 58.3% | |
| Transporter, technician | 41 | 19.4% | |
| Transporter, intern | 0 | .0% | |
| Received supportive actions | 47 | 22.3% | |
| Occurrence of peculiar events | 10 | 4.7% | |
| intubation | 52 | 24.6% | |
| Appropriate tracheal intubation | 37 | 61.7% | |
| Vascular accessibility | 195 | 92.4% | |
| 167 | 79.1% | ||
| Neonate’s general condition | unstable | 44 | 20.9% |
| hypothermia | 11 | 5.2% | |
| cyanosis | 31 | 14.7% | |
| Oxygen reception | 137 | 64.9% | |
| Ambu bag | 22 | 10.4% | |
| therachetube10 (therachetube10) | 24 | 11.4% | |
| Laryngoscope usage | 2 | .9% | |
| Suction usage | 9 | 4.3% | |
| bagsize (bagsize) | 64 | 30.3% | |
| prssuresoopap (prssuresoopap) | 13 | 6.2% | |
| mask | 21 | 10.0% | |
| Participation of transporter in CPR workshops | 142 | 75.1% | |
| Transporting vehicle | incubator | 200 | 94.8% |
| 4 | 1.9% | ||
| 7 | 3.3% | ||
| Hospital type | governmental | 114 | 54.0% |
| 65 | 30.8% | ||
| 32 | 15.2% | ||
| Classification of numbers of births | 1 | 188 | 89.1% |
| 23 | 10.9% | ||
| Problem type | internal | 98 | 50.5% |
| 96 | 49.5% | ||
| receptionist | attend | 83 | 43.0% |
| 85 | 44.0% | ||
| 25 | 13.0% | ||
| Birth type | natural | 53 | 25.1% |
| 158 | 74.9% | ||
| Previous hospitalization unit | neonatal | 51 | 24.6% |
| 40 | 19.3% | ||
| 115 | 55.6% | ||
| 1 | .5% | ||
| Surfactant prescription | 32 | 15.5% | |
| hopshystory (hopshystory) | 3 | 1.4% | |
Table 2: Quantitative variables of subjects
| Mean | S.D. | Max. | Min. | |
| Pregnancy duration (weeks) | 33.60 | 7.24 | 41.00 | .00 |
| Weight on birth (grams) | 2446.24 | 888.27 | 5000.00 | 700.00 |
| 1-minute Apgar | 7.32 | 1.85 | 9.00 | .00 |
| 5-minuts Apgar | 8.55 | 1.61 | 10.00 | .00 |
| Mother’s Age (years) | 27.32 | 5.68 | 47.00 | 15.00 |
| Number of births | 1.59 | .81 | 6.00 | 1.00 |
| l (l) | 1.39 | .80 | 6.00 | .00 |
| abortion | .32 | .63 | 3.00 | .00 |
| Number of pregnancies | 1.75 | .98 | 6.00 | 1.00 |
| Number of administered surfactants | 1.15 | .46 | 3.00 | 1.00 |
| Transportation duration (hours) | 81.98 | 106.20 | 540.00 | 15.00 |
|
Newborn’s age (hours) |
798.00 | 8797.41 | 126048.00 | 1.00 |
People accompanying the newborn were physicians in 58 cases (27.5%), nurses in 123 cases (58.5%), and surgery room or anesthesiology technicians in 41 cases (19.4%).
52 (24.6%) cases had tracheal tube and 159 (75.4%) did not during transportation.
From those who had tracheal tube in 38 cases (71.1%) it was placed in an appropriate position.
195 newborns (92.4%) had vascular access device during transportation.
167 (79.1%) were in stable conditions at the time of arrival to NICU while 11 (5.2%) and 31 (14.7%) cases were hypothermic and had cyanosis, respectively, making a proportion of 20.9% (44 cases) of all subjects.
137 newborns (64.9%) received oxygen during transportation. In 22 cases (10.4) a bag of air conditioner was used and laryngoscope was implemented for 2 subjects (0.9%) for intubation.
From all participants 142 stated that they had participated in resuscitation workshops while 47 mentioned they had not who are 62.8% and 20.7% respectively. The rest of participants did not have any information regarding this item.
91 transportation institute were governmental and 91 were private, making 43.1% each.
Almost all cases (99, equivalent to 94.2%) were transported via incubators.
119 newborns (56.4%) were males and the rest were females.
112 (53.1%) of all hospitals were governmental, 68 (32.2%) were private, and rest were from other organizations such as social security organization, armed forces, etc.
90% of pregnancies (190 cases) were singlet and 10% (21 cases) were multiplets.
As for 1-minute Apgar score, there was no information about 75 cases (35.5%) of all. Apgar scores of 5 subjects were 3 or lower. This value for 25 cases (11.9%) was 3 or between 3 and 7, and for 106 subjects (50.3%) it was 7 or higher.
From 132 cases who had 5-minute Apgar score, 2 cases (1%) had a score of 3 or lower, 10 (4.7%) had a score between 4 and 7, and the rest (120 cases, equivalent to 56.9%) were higher than 7.
The reasons for transportation were internal and surgical problems in, respectively, 109 (51.7%) and 102 (48.3%).
The receptionists were attending physicians (internal and surgery), fellows, and residents in 87 (42.2%), 94 (44.5%), and 30 (14.2%) cases respectively.
The birth types were natural in 53 cases (25.1%) and cesarean in 158 (74.9%) cases.
The transported newborns to Mofid hospital’s NICU had been hospitalized previously in neonatal units, nurseries, and NICUs in, respectively, 51 (24.2%), 40 (19%), and 115 (54.5%) cases.
In 179 cases (84.8%) surfactant had not been prescribed in their previous medical center while 32 cases (15.2%) were injected.
From all patients only 3 (1.4%) had the experience of being hospitalized in Mofid hospital’s NICU and the rest were all new to the situations.
The cities of birth were Tehran, Qom, Arak, and Karaj in, respectively, 146 (70.2%), 8 (3.8%), 9 (4.3%), and 9 (4.3%) cases.
As for initial determination of the disease, the most common referral reason was respiratory dystrophy with 83 occurrences and the followings were prematurity, esophageal atresia, and diaphragmatic hernia with 22, 17, and 9 incidences.
The mean and standard deviation of newborns’ ages were 189.21 and 350 hours. The minimum and maximum values were one hour and 90 days respectively. The most frequent value (Mode) was 24 hours.
The mean and S.D. for weight were 2446 and 888.26 grams and the minimum and maximum values were 700 and 5000 grams.
Mean and S.D. were 27.32 and 5.68 years for mothers’ ages. The exterma were 15 and 47 years for this item.
Shortest and longest transportation time were 15 and 540 minutes (mean = 81.97 minutes).
25 and 41 weeks were the exterma values for pregnancy length with a mean of 34.66.
There were no significant relation between the general wellbeing of newborns and the person who is responsible for transportation (physician, nurse, or technician) (graph 1). In unstable cases the percentage of the presence of a physician were higher than two others. When analyzing the relation of general wellbeing of the newborns with the participation of the person accompanying the subject during transportation in CPR workshops, no significant one was found.
In addition there was no significant difference between transportation duration and birth type in both groups (stable and unstable).
The relative frequency of stable overall conditions in newborns transported via governmental ambulances was higher, however its difference with other ambulances was not significant (graph 2).
In those incidents in which a physician accompanied the subject the relative frequency of the appropriate intubation was higher. This value was also higher with those cases transported by someone who had passed CPR workshops or a private ambulance, however the differences were not statistically significant. There were no significant difference between the types of the center (governmental, private, etc.) with respect to the levels of participating in CPR workshops.
In unstable cases a higher percentage had internal problems, however this was not significant when compared to the group with stable overall conditions.
A higher proportion of newborns who were transported from private hospitals had received surfactant, nevertheless the difference was insignificant. Furthermore, prescription of surfactant was insignificantly higher in cases with internal problems compared to those with surgical problems.
The mean weight and the mothers’ age were lower in the group prescribed with surfactant. Both these relations were found to be significant.
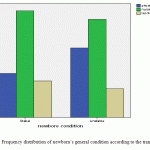 |
Figure 1: Frequency distribution of newborn’s general condition according to the transporter |
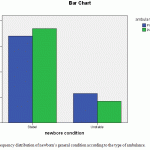 |
Figure 2: Frequency distribution of newborn’s general condition according to the type of ambulance |
Discussion
Generally it has been shown in several studies that, like preterm newborns, term newborns also may face serious dangers 121314 making transportation a necessity in a way that the mean pregnancy duration in our study was 34.66 weeks (the exterma were 25 and 41), and 33.79, 35.8, and 31.8, respectively, in three other studies in Sari 15, Shiraz Zeinabieh 16, and Tehran 17.
The mean duration of hospitalization were less than 24 hours in studies in Sari and Tehran while in our research this was elevated to 89.21 hours suggesting an increase in neonatal units in different healthcare centers. The infant respiratory distress syndrome with 5.65% in Sari and 7.72% in a previous study in Tehran decreased to 5.39% 1517. This and the fact that 5.54% and 2.24% of transported cases were previously hospitalized in, respectively, NICU and neonatal units suggest an increase in the number of care centers.
Augmentation of transported newborns diagnosed with surgery in our study from 73.22% to 3.48% is a sign of elevated life expectancy in these patients and active surgery centers and this means a relative upturn in respiratory distress cases’ outcomes in recent years.
Treatment and stabilization of overall condition of newborns before transportation is of high importance 18. In a study in Sari 1.10% and 2.39% of subjects were hypothermic and cyanotic respectively and neither groups had been prescribed with surfactant 15. However in our study 2.5% of cases were hypothermic and 7.15% were cyanotic and in a research in Canada the proportion of hypothermia was 2.25% 19. Considering the surfactant prescription in 2.15% of transported cases in our study it can be perceived as a relative improvement of diagnosing and treatment equipment.
In our results it was shown that the mean duration of pregnancy and the mean weight were lower in the group which received surfactant. This was statistically significant in both aspects. However, there were no significant relation between patients with internal and surgical problems with respect to prescription of this medicine. Though this value was higher in internal patients it could be due to the fact that the surgical patients encounter many problems such as failure, respiratory distress, etc. 20 which make the prescription of surfactant inevitable.
As for the transportation conditions, 10 years ago in Tehran 17 84.36% and in a study in Sari 15 7.79% and 3.94% of cases in our investigation were transported via portable incubators and all cases had CPR bags. Transportation duration increased in our study to 81±97 minutes when compared to 10 years ago in which this value was 46±17 minutes. This is justifiable considering that 8.29% of subjects were transported from another city to Tehran.
In the study of Sari 9.12% of subjects had tracheal tube and 7.2% of these cases had inappropriate positioning. In our study these values were 6.24% and 6.6% respectively. The frequency of appropriate intubation was higher when the transportation was carried out by a physician or someone who had passed CPR workshops. However statistical insignificance of the relation necessitates further investigations with larger sample populations and more information about participating in CPR workshops.
Transportation of newborns to NICUs requires a trained team. Several studies demonstrated that transportation side effects such as hypothermia and acidosis and some events such as tracheal tube loss is higher when an amateur team is responsible 21 22. In the previous study in Tehran in 9.78% of incidents a nurse and in 1.21% an intern accompanied the patient 17. In Sari 4.32% of cases were conveyed by a nurse and 6.67% by an intern and a nurse 15. These proportions were 5.27%, 5.58%, and 4.19% for, respectively, physicians, nurses, and technicians in our study.
Conclusion
However the percentage of physician participation in unstable cases was higher in our study, there were no significant relation between the accompanying person and stability of the patient. This suggested that appropriate training, and CPR and retraining courses are more effective. This is in agreement with the American neonatology society’s recommendation stating that one of the members of the team must be an skilled nurse with 5 years of working experience.
References
- Tangcharoensathien V, Faramnuayphol P, Teokul W, Bundhamcharoen K. A critical assessment of mortality statistics in Thailand : potential for improvements. 2006;026310(05).
- Machado CJ, Hill K. Maternal, neonatal and community factors influencing neonatal mortality in Brazil. J Biosoc Sci. 2005;37(2):193-208. Available at: http://www.ncbi.nlm.nih.gov/pubmed/15768774. Accessed May 1, 2015.
- Onayade AA, Akanbi OO, Okunola HA, Oyeniyi CF, Togun OO, Sule SS. Birth preparedness and emergency readiness plans of antenatal clinic attendees in Ile-ife, Nigeria. Niger Postgrad Med J. 2010;17(1):30-9. Available at: http://www.ncbi.nlm.nih.gov/pubmed/20348980. Accessed April 30, 2015.
- Hood JL, Cross A, Hulka B, Lawson EE. Effectiveness of the neonatal transport team. Crit Care Med. 1983;11(6):419-23. Available at: http://www.ncbi.nlm.nih.gov/pubmed/6851597. Accessed May 1, 2015.
- Joseph M, Hageman JR. Neonatal transport: a 3-day-old neonate with hypothermia, respiratory distress, lethargy and poor feeding. J Perinatol. 2002;22(6):506-9. doi:10.1038/sj.jp.7210755.
- Mmbaga BT, Lie RT, Kibiki GS, Olomi R, Kvåle G, Daltveit AK. Transfer of newborns to neonatal care unit: a registry based study in Northern Tanzania. BMC Pregnancy Childbirth. 2011;11:68. doi:10.1186/1471-2393-11-68.
- Mamunur Rashid AKM, Habibur Rasul CH, Hafiz SM. Neonatal mortality: a scenario in a tertiary level hospital of a developing country. Pediatr Rep. 2010;2(1):e9. doi:10.4081/pr.2010.e9.
- Storrs CN, Taylor MR. Transport of sick newborn babies. Br Med J. 1970;3(5718):328-32. Available at: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=1701480&tool=pmcentrez&rendertype=abstract. Accessed May 1, 2015.
- Vieira ALP, Santos AMN dos, Okuyama MK, Miyoshi MH, Almeida MFB de, Guinsburg R. Predictive score for clinical complications during intra-hospital transports of infants treated in a neonatal unit. Clinics (Sao Paulo). 2011;66(4):573-7. Available at: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3093786&tool=pmcentrez&rendertype=abstract. Accessed May 1, 2015.
- Romanzeira JCF, Sarinho SW. Quality Assessment of Neonatal Transport performed by the Mobile Emergency Medical Services (SAMU). J Pediatr (Rio J). 2015. doi:10.1016/j.jped.2014.10.006.
- Field D, Milligan D, Skeoch C, Stephenson T. Neonatal transport: time to change? Arch Dis Child Fetal Neonatal Ed. 1997;76(1):F1-2. Available at: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=1720608&tool=pmcentrez&rendertype=abstract. Accessed May 1, 2015.
- Cuna A, Hakima L, Tseng Y-A, et al. Clinical dilemma of positive histologic chorioamnionitis in term newborn. Front Pediatr. 2014;2:27. doi:10.3389/fped.2014.00027.
- Hazza IA, Ghandour MS, Almardini RI, Haddad RE, Salaita GM. Hypercalcemia, hypercalciuria and nephrocalcinosis in a breast-fed term newborn: a rare presentation. Saudi J Kidney Dis Transpl. 2014;25(4):849-53. Available at: http://www.ncbi.nlm.nih.gov/pubmed/24969200. Accessed May 1, 2015.
- Ballou JF, Gray BP, Mancuso P. Bradycardia in a term newborn. J Pediatr Health Care. 2014;28(5):456-60. doi:10.1016/j.pedhc.2014.01.004.
- Nakhshab M, Vosughi E. The Condition of Neonatal Transport to NICU in Mazandaran. J Maz Univ Med Sci 2010; 20(78) 50-57 (Persian). 2010:49-57.
- Arianpour S, Sabet S. Study of factors effective on neonatal transport, NICU In Zeinabie hospital in Shiraz. Med Res. 2003;3(1):22-24.
- Kazemian M, Fakhraee S, Zonouzi F. Neonatal Transport in Tehran: a Cause for much concern. Arch Iran Med. 2004;4(7):256-259.
- Dulkerian SJ, Douglas WP, Taylor RM. Redirecting treatment during neonatal transport. J Perinat Neonatal Nurs. 25(2):111-4. doi:10.1097/JPN.0b013e31821a20ab.
- Khurshid F, Lee K-S, McNamara PJ, Whyte H, Mak W. Lessons learned during implementation of therapeutic hypothermia for neonatal hypoxic ischemic encephalopathy in a regional transport program in Ontario. Paediatr Child Health. 2011;16(3):153-6. Available at: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3077305&tool=pmcentrez&rendertype=abstract. Accessed May 1, 2015.
- Catré D, Lopes MF, Madrigal A, et al. Predictors of major postoperative complications in neonatal surgery. Rev Col Bras Cir. 40(5):363-9. Available at: http://www.ncbi.nlm.nih.gov/pubmed/24573583. Accessed May 1, 2015.
- Lynch TF, Kugler L, Niedziela J. Saving our smallest patients. J Healthc Prot Manage. 2014;30(2):72-82. Available at: http://www.ncbi.nlm.nih.gov/pubmed/25181794. Accessed May 1, 2015.
- Fairchild K, Sokora D, Scott J, Zanelli S. Therapeutic hypothermia on neonatal transport: 4-year experience in a single NICU. J Perinatol. 2010;30(5):324-9. doi:10.1038/jp.2009.168.

This work is licensed under a Creative Commons Attribution 4.0 International License.





