How to Cite | Publication History | PlumX Article Matrix
P. I Aziba1* , Tari R. Idumange1, Senjobi, C. T2
, Tari R. Idumange1, Senjobi, C. T2 , Adeniyi-Akee M3
, Adeniyi-Akee M3 and Adedokun Oluwasegun4
and Adedokun Oluwasegun4
1Department of Pharmacology and Toxicology, Dora Akunyili College of Pharmacy Igbinedion University, Okada Olabisi Onabanjo University, Ago Iwoye Nigeria.
2Department of Plant science, Igbinedion University, olabisi onabanjo university Ago Iwoye. Nigeria.
3Department of Pharmaceutical Chemistry, Igbinedion University, Okada Olabisi Onabanjo University, Ago Iwoye Nigeria.
4Department of Pharmacognosy, Igbinedion University, Okada Olabisi Onabanjo University, Ago Iwoye Nigeria.
Corresponding Author E-mail: peteraziba1@gmail.com
DOI : http://dx.doi.org/10.13005/bbra/2991
ABSTRACT:
Experimental paralysis was induced intramuscularly (i.m) in rats , using Suxamethonium(1.08mg/kg ) , Decamethonium (1.08mg/kg ) in normotensive rats weighing150-180g±2.5g (n=8).Various concentrations of these drugs ranging from (0.36—1.08mg/kg) were used , in order to assess at what concentrations will induced spastic paralysis sustained without death. Similarly, dose response concentrations effect was examined and the onset of action( ie time taken to observe paralysis and manifestation of pain and death was recorded. In some experiments, equimolar concentrations of Suxamethonium(1.08mg/kg) and Decamethonium(1.08mg/kg) was used to assess reaction time(RT) and potency of the agents. Thereafter the actions of Calcium Channel blockers (CCB), Diltiazem ( DTZ) and verapamil(VE) were studied in separate experiments. Anticholinesterase agent(AchE) in combination with Atropine a known antimuscarinic agent(AchE ) and investigated their actions on induced paralysis. The results obtained in these studies showed that CCB produced a significant potentiation of spastic paralysis on Suxamethonium induced paralysis but non reversal effect with Decamethonium , while AchE in combination ATR showed a reversal effect on paralysis induced by these agents in the concentrations used in his study. The aim of the study was to see interaction of these agents on sustained experimental paralysis in rodent.
KEYWORDS: Anticholinesterases; Calcium Channel blockers; Neuromuscular depolarizing; Paralysis
Download this article as:| Copy the following to cite this article: Aziba P. I, Idumange T. R, Senjobi, C. T, Akee M. A, Oluwasegun A. Studies on the Actions of Calcium Channel Blockers, Anticholinesterases Agents on Experimentally Induced Spastic Paralysis in Normotensive Rats. Biosci Biotech Res Asia 2022;19(2). |
| Copy the following to cite this URL: Aziba P. I, Idumange T. R, Senjobi, C. T, Akee M. A, Oluwasegun A. Studies on the Actions of Calcium Channel Blockers, Anticholinesterases Agents on Experimentally Induced Spastic Paralysis in Normotensive Rats. Biosci Biotech Res Asia 2022;19(2). Available from: https://bit.ly/3MJadw8 |
Introduction
The neuromuscular junction(NMJ) is a synaptic connection between the terminal end of a motor nerve and muscle(Skeletal),It is the site for transmission of action potential from nerve to muscles.it is also the site for many diseases and a site for many drugs.[Jimsheieishvili , et al 2020]. Drugs or agents that act at this sites are either depolarizing and non- depolarizing .The depolarizing neuromuscular blockers act by blocking neurotransmission at NMJ, causing paralysis of the affected skeletal muscle at the post synaptic acetylcholine(Nm) receptors ((Dlines, et al 2018.) The present studies investigated the actions of Calcium channel Blockers(CCB) Diltiazem (DTZ),Verapamil (VER) Cook , et al 2020.), and anticholinesterase agent Pyridostigmine(PYT), in combination with atropine(ATR) a known anti -muscarinic agents on Decamethonium (Deca) Suxamethonium (suxa) induced experimental paralysis in Rats. Neuromuscular blocking drugs are also drugs that induce paralysis of the skeletal muscle, hence they are also known as skeletal muscle relaxants [Feldman, et al 1996.),are used primarily as adjuncts during general anesthesia to optimize surgical conditions and to facilitate endotracheal intubation in order to ensure adequate ventilation.
Spastic paralysis refers to a condition where the tone of muscles is raised and at the same time muscles are weak stiff and weak (Michael, et al 2020). The most common causes involve diseases that damage the descending tracts anywhere along their long course from the brain to the spinal cord. Due to damage to the controlling areas of the brain of the descending tracts, muscle tone increases in an unchecked manner and muscles are stiff or, “spastic.” Examples include stroke, which affects the cortex of the brain or the brainstem. This is also called an “upper motor neuron (UMN)” type of weakness in technical parlance. Due to the increased tone, deep tendon reflexes will be exaggerated [Kraynack, et al 1983).While Flaccid paralysis is a condition where the tone of the muscles is reduced and the muscles are weak. This could be due to a disease of the final cells or circuits in the spinal cord that effect the tone (polio, ALS) or diseases of the nerves that supply the muscles. This is also called a “lower motor neuron (LMN)” type of weakness in technical parlance. Due to the reduced tone, the tendon reflexes will be suppressed [Mathew P.B 1984].
Materials and Method
Drugs Used
Atropine (EMPL), Suxamethonium chloride ampoule (Rotex Medical), Decamethonium salts (Sigma), Verapamil (TEVA UK Ltd), Diltiazem (EthyPharm), Predetermine (comMostone) Drug dilutions of appropriate concentrations were used.
Animal
Sprague Dawley rats used were obtained from the Animal House, Department of Pharmacology, College of Pharmacy, Igbinedion University, Okada, Edo State. Their weights ranged from 150 – 180g ±2.5. Animals were maintained on standard animal pellets and water ad libitum. The experiment was carried out in strict compliance with the National Institute of Health, 1985 and ethical approval was given by the university ethics committee. (IUOETH/2020/15FPM).
Experimental Procedures
Normotensive Sprague Dawley rats were administered intramuscularly with 0.36mg/kg of Suxa (i.m). The rats were then observed for signs of spastic paralysis. The dose was doubled on another set of rats (0.72rmg/kg) and tripled on the third set of rats (1.08mg/kg n=8) until signs of spastic paralysis could be observed. The reaction time was noted. The same procedure was carried out using Deca.
In some experiments, equimolar concentrations of Suxa and Deca were used in this study. Rats were administered Suxa at 1.08mg/kg (i.m) and observed for signs of spastic paralysis. The procedure was then repeated for Deca at the same concentration (1.08mg/kg (n=8) Duration of action was noted to assess the action of the drugs.
Rats were administered 6.67mg/kg of verapamil 15 minutes prior to administration of 0.36mg/kg Deca (i.m). Reaction time was noted, .
he procedure was then repeated using 0.36mg/kg(n=8) and 1.08mg/kg of Suxa.
In this experiment, rats were administered 5mg/kg of diltiazem 15 minutes prior to administration of 1.08mg/kg of Suxa i.m. The rats were observed for signs of spastic paralysis and reaction times were noted. The procedure was then repeated using 1.08mg/kg of deca.
Rats were administered 1.08mg/kg(n=8) of Suxa i.m, . Once the signs of spastic paralysis were manifested, the rats were then immediately administered 5mg/kg of PYR and 18µg/kg of Atr (n=8). the frequency of paralysis and if the paralysis was ultimately reversed. The same procedure was repeated using 1.08mg/kg of Deca and 5mg/kg of PYR in combination with18ug/kg ATR.
Results
The results obtained in this study were presented in a bar chart.
Using equal dose (1.08mg/kg) of suxa and deca
The reaction time of suxa was 4 minutes, compared to deca which was 13 minutes. (Fig. 1) This shows that suxa is more potent than deca. (Chart 1).
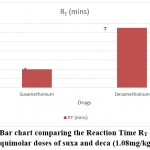 |
Figure 1: Bar chart comparing the Reaction Time RT (mins) for equimolar doses of Suxamethonium and Decamethonium (1.08mg/kg). |
SEM ±0.5 (T), n=8, RT = Reaction time
Interaction between CCB (VE and DTZ) and Suxa/Deca
VE significantly enhanced the neuromuscular blocking activities of Suxa and Deca, shown in the shorter reaction time (2 mins for deca and less than 30 secs for suxa). (Fig below).
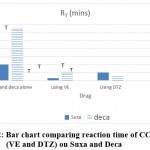 |
Figure 2: Bar chart comparing reaction time of CCB (VE and DTZ) on Suxamethonium and Decamethonium. |
P< 0.5 , n=8, RT = Reaction time
Using DTZ, there was also a significant potentiation of spastic paralysis effect as shown in the shorter reaction time (1 minute for deca and 2 mins for suxa). Changes in spastic paralysis were represented as reaction time (mins).
Interaction between PYR+Atr and Suxa/Deca
PYR+Atr slowed the neuromuscular blocking activities of Suxa, but did not produce reversal of spastic paralysis, while it significantly inhibited the neuromuscular blocking activities of deca, (Fig 3).
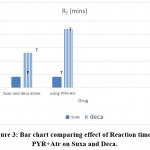 |
Figure 3: Bar chart comparing effect of Reaction time of PYR+Atr on Suxamethonium and Decamethonium. |
P,<0.5 (T),( n=8), RT = Reaction time
Changes in spastic paralysis were represented as reaction time.
Table 1: Show Decamethonium that elicited a paralysis effect without causing death (see Table 1 below).
| Drug | Dose (mg/kg) | To (mins) | RT (mins) | No. of Rats (n) |
| Suxamethonium | 0.36 | 00.00 | 00.01 ±0.5 | 8 |
| Suxamethonium | 0.72 | 00.30 | 00.31 ±0.5 | 8 |
| Suxamethonium | 1.08 | 01.00 | 01.04 ±0.5 | 8 |
| Decamethonium | 0.36 | 00.00 | 00.04 ±0.5 | 8 |
| Decamethonium | 0.72 | 00.30 | 00.38 ±0.5 | 8 |
| Decamethonium | 1.08 | 01.00 | 01.13 ±0.5 | 8 |
Strength of Suxamethonium and Decamethonium – 0.5mg/ml.
Concentration of Suxamethonium that caused paralysis = 1.08 mg/kg
Concentration of Decamethonium that caused paralysis = 1.08 mg/kg
P ˂ 0.05, n = (8), Time of administration, RT = Reaction time, n = no. of rats observed in experiment, Standard Error (S.E) ±0.5
Table 2: Show the dose of suxamethonium that elicited a paralysis effect without causing death (see Table 2 below).
| Dose (µg) | To (mins) | RT (mins) | Death (mins) | No. of Rats (n) |
| 50 µg | 00.00 | 00.11 ±0.5 | No | 8 |
| 75 µg | 00.00 | 00.01 ±0.5 | 2 | 8 |
| 100 µg | 00.00 | 00.01 ±0.5 | 5 | 8 |
| 5000 µg | 00.00 | 00.01 ±0.5 | 8 | 8 |
P ˂ 0.05, n = (8), time of injection, RT = Reaction time, n = no. of rats observed in experiment, P< ±0.5
Table 3: Shows the potency of equimolar concentrations (1.08mg/kg) of Suxamethonium and Decamethonium.
| Drug | Dose (mg/kg) | To (mins) | RT (mins) | No. of rats (n) |
| Decamethonium | 1.08 | 00.00 | 13.0 ±0.5 | 8 |
| Suxamethonium | 1.08 | 4 | 00.01 ±0.5 | 8 |
P ˂ 0.05, n = (8), time of administration, RT = Reaction time, n = no. of rats observed in experiment, Standard Error (S.E) ±0.5
Table 4: Shows effect that Verapamil (6.67mg/kg) on spastic paralysis induced by Suxamethonium and Decamethonium.
| Drug | Dose (mg/kg) | To (mins) | RT (mins) | Duration of action | No. of Rats (n) |
| Decamethonium | 0.36 | 00.00 | 00.02 | 8 mins ±0.5 | 8 |
| Suxamethonium | 0.36 | 00.00 | 00.01 | 15 mins ±0.5 | 8 |
| Suxamethonium | 1.08 | 00.00 | 00.00 (<30 secs) | 2 mins ±0.5 | 8 |
P ˂ 0.05, n = (8), To = time of injection, RT = Reaction time, n = 8 , Standard Error (S.E) ±0.5
Table 5: Shows the effect of Verapamil (6.67and13.34mg/g at different concentrations on spastic paralysis induced by Suxamethonium and Decamethonium.
| Drug | Dose (mg/kg) | Dose of verapamil (mg/kg) | To
(mins) |
RT (mins) | No. of Rats (n) |
| Suxamethonium | 0.36 | 6.67
|
00.00 | 4.0 ±0.5 | 8 |
| Decamethonium | 0.36 | 13.34
|
00.00 | 00.05 ±0.5 | 8 |
P ˂ 0.05, n = (8), time of administration, RT = Reaction time, n = 8. of rats , Standard Error (S.E) ±0.5.
Table 6: The show the effect of diltiazem 5mg/kg in equimolar concentrations (1.08mg/kg) of Suxamethonium and Decamethonium in rats.
| Drug | Dose
(mg/kg) |
To
(mins) |
RT (mins) | No. of Rats (n) | Duration of action (mins) |
| Suxamethonium | 1.08 | 00.00 | 4.0±0.5 | 8 | 7 |
| Decamethonium | 1.08 | 00.00 | 13 ±0.5 | 8 | 10 |
P ˂ 0.05, n = (8), time of injection, RT = Reaction time, n = no. of rats observed in experiment, P< ±0.
Table 7: Show the effect pyridostigmine (5mg/kg) in combination with atropine (18µg/kg) on Suxamethonium and Decamethonium induced paralysis.
| DRUG | Suxamethonium | Decamethonium |
| Dose (mg/kg) | 1.08 | 1.08 |
| 00.00 | 00.00 | |
| 00.03 | 00.06 | |
| 00.03 ±0.5 | 00.06 ±0.5 | |
| PYR+Atr (mins) | 00.03 ±0.5 | 00.06 ±0.5 |
| RT of PYR+Atr (mins) | 00.04 ±0.5 | 00.22 ±0.5 |
| No. of Rats (n) | 8 | 8 |
P ˂ 0.05, n = (8),
Time of injection, RT = Reaction time, n = 8. of rats observed in experiment, Standard Error (S.E) ± 0.5.
Discussion
Skeletal muscle relaxants, neuromuscular blocking drugs. and, Spasmolytic generally act at the gamma-aminobutyric acid (GABA) receptors as an agonist, to facilitate the spinal inhibition of motor neurons. Clinically, these classes of drugs can be used to treat spasticity due to disease conditions such as cerebral palsy, multiple sclerosis and stroke. Some other direct-acting muscle relaxants suck as botulinum toxin, can induce flaccid paralysis[Mckinon, et al, 2013]
The actions of these agents( CCb), Anticholinesterases and in combination with a known muscarinic agents(PYR+ATR) in the concentrations used in the study, the results obtained are discussed as follows generally, neuromuscular blocking agents that act as agonists to acetylcholine(Nm) at the neuromuscular junction, causing stimulation of the muscle cell and occupying the receptor sites(postsynaptic) preventing it from it from repolarizing and results to paralysis
In some of the results in which loss of animal could be due to excessive paralysis thereby muscle paralysis.The results indicated that Suxa in 4minutes paralysis occurred while with Deca sustained paralysis was after 13minutes indicating that onset of action was faster with Suxa than Deca. Results in which effect of Suxa was potentiated by CCB will indicate facilitation of calcium which is necessary for muscle contractions, but the non reversal.effect Deca in the study in which anticholinesterases in combination with anti muscarinic agents can be explained ACHE drugs such as neostigmine, which prevent the destruction by cholinesterase of acetylcholine release at the nerve endings enable concentration of ach build up and thereby reduce the effect of NM Blocking agents,
The time-dependent study in this work, in which the results indicated that the paralysis was induced in Suxa in 4 minutes and in Deca in 13 minutes shows that Suxa is more potent than Deca. The equimolar study of concentration of drug use is to establish the potencies of the drugs in order to explain their interaction or effect on spastic paralysis by suxa and Deca. (% of suxa = 23.5%, % of deca = 76.5%)
Results show that CCB produce significant potentiation of the spastic paralysis effects of Suxa and Deca but in differing degrees (Fig 4). Diltiazem and verapamil caused a concentration dependent potentiation of paralysis. These
effects are similar to those reported previously using rats phrenic nerve muscle preparation. (Kraynack, et al, 1983).
The CCBs are drugs that blocks influx of Ca2+ by limiting the presence of this ion, thereby enhancing paralysis as reported. If paralysis is caused by blocking of transmission at the NMJ, it is important to see the interaction between CCB and deca/suxa. In this study, CCB (VE & DTZ) showed potentiatory effects on spastic paralysis induced by Suxa and Deca, which indicated the frequency of spasticity (personal observation).
The use of PYR + Atr was to assess the action of this drug at the NMJ. Since we know that the neurotransmitter released at the NMJ is ACh, it therefore follows that we investigated the action of PYR+Atr, to assess if Acetylcholinesterase (Enzyme that hydrolyzes ACh) would be inhibited, thus leading to an increase in ACh at the NMJ and reversing the spastic paralysis effect (DLines, et al 2018) of suxa and deca. But our findings did not show the expected action. Hence it did not reverse the action of suxa, however, it did reverse the action of deca. That can be explained that the reaction of suxa is predominantly at the nicotinic receptors but Atropine works predominantly on the muscarinic receptors.
PYR is an anticholinesterase that increase the effect of acetylcholine by preventing cholinesterase in this action. The use of atropine in this combination would suggest that nicotinic receptors may be involved in spastic paralysis, but muscarinic receptors are predominant receptors at the NMJ. Hence this accounts for the non-reversal of ACh. In conclusion, the results of this study indicated that CCBs (VE and DTZ) had a potentiatory effect on spastic paralysis induced by suxa and deca, while PYR+Atr had an inhibitory effect on deca but showed no effect on suxa (Kraynack BJ et al, 1983.).
Acknowledgement
Author wishes to thank Mr Akpan Eyibo , for his Technical support during the study.
Conflict of Interest
There is no conflict of Interest.
Funding Sources
There is no funding sourece.
References
- Jimsheleleishvili S, Marwana , k, Sherman AL 2021 Instat Pearls (internet) treasure Island Pub Med.ncbi.nlm.gov.
- Feldman S Kara L, Drug interaction with neuromuscular blockers. Drug saf 1996 vol 5 (4) 261 -73 (pubmed).
CrossRef - Michael, A Gropper; In Miller Anaesthesia 2020: Pharmacology of Neuromuscular block. Neuromuscular blocking agents –an overview .science direct.
- Neuromuscular blocking asgents(NMDA) are used in Clinical Practice for condition requiring paralysis such as rapid sequence intubation .Science Direct 2018.
- D. Lines Chris ,Hani, Baragwanath. Academic hospital ; neuromuscular blocking agents- when is the block deep enough? And hiow to safely reverse the neuromuscular block DOI:4102/ Safp.vol 60:4 2018 .South Africa Family Pratice.
CrossRef - Kraynack BJ, Lawson NN, Gintautas J, e-Jay H+ effects of verapamil on muscle and twitch responses. Anaesthesia and Analgesia 1983; 62: 8
CrossRef - Rodriguez-beato Fy. Jesus o. ;Physiology. Deep Tendon reflex –stat Pearls –NCBI.
- Mckinon, W.the accuracy of subjective clinical assessment of the patellar reflex.Muscle Nerve 2013 jan 47(1) 81-8 (pubmed) ref list.
CrossRef

This work is licensed under a Creative Commons Attribution 4.0 International License.





